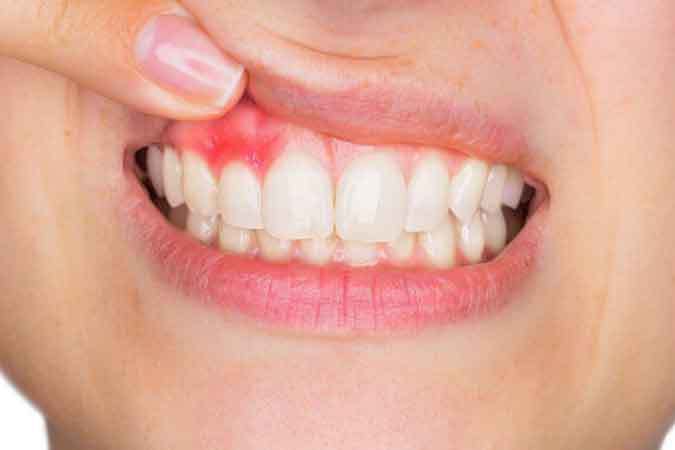
Gum recession is when the gum tissue pulls back from the tooth, exposing the root — and once it happens, it does not grow back on its own. The good news: it can be stopped at almost any stage, and in earlier stages (Miller class I and II) surgical root coverage can restore close to 100%. This guide explains the six causes we see most often in our Brooklyn practice, how dentists grade severity using the Miller classification, and what treatment looks like at each stage.
What “receding gums” actually means
Healthy gum tissue (the gingiva) sits as a thin pink collar around the neck of each tooth, covering the root and bone underneath. When the gums recede, that collar migrates downward (on lowers) or upward (on uppers) and the cementum-covered root surface becomes visible. Cementum is softer than enamel, more porous, and not built to be exposed — which is why recession brings new sensitivity to cold, sweet, or air, and why exposed roots develop cavities much faster than the crown.
Recession can affect a single tooth (often a lower front tooth or canine) or be generalized across the whole mouth. It is frequently asymmetric — the side you brush harder, the side you sleep on, or the side where a tooth sits outside the arch shows it first. Gum tissue does not regenerate on its own once lost; true coverage requires either composite bonding to mask it or a surgical graft to restore it.
Dr. Natalia Blazhkevich has practiced general and cosmetic dentistry at our Sheepshead Bay office since 2018 and sees recession every week. The treatment path depends entirely on which of the six underlying causes is driving the problem.
The 6 causes of gum recession
1. Aggressive brushing (the most common cause we see)
This is by far the leading driver of recession in patients who do not have gum disease. The culprits: a hard-bristled brush, heavy pressure (most people use 2–3 times what they need), a sawing side-to-side motion, and abrasive whitening pastes used aggressively for years. The classic appearance is a V-shaped notch at the gum line, often paired with wedge-shaped root erosion called abfraction, showing up first on canines and premolars on the dominant-hand side.
The fix requires retraining: a soft or extra-soft brush (electric with a pressure sensor is the fastest way to learn), light pressure, and the modified Bass technique — bristles at 45° to the gum line, short gentle vibrations, no scrubbing. Reserve in-office whitening for one-time cosmetic boosts instead of grinding away enamel with abrasive paste every morning.
2. Periodontitis (gum disease)
Recession driven by periodontitis looks different: more generalized tissue loss, often with bleeding, persistent bad breath, and in advanced cases looseness. The mechanism is bacterial — plaque biofilm matures into an infection that erodes both gum attachment and the underlying alveolar bone. Bone loss is the key distinction, and it is irreversible without specialized surgical procedures.
Treatment is entirely different from brushing-related recession: scaling and root planing under local anesthesia, sometimes locally placed antibiotics, 3-month periodontal maintenance, and in moderate-to-severe cases referral for pocket reduction. The full protocol is on our gum disease treatment in Brooklyn page. If your recession comes with bleeding and bad breath, periodontitis is the first thing to rule out.
3. Genetics and thin gum biotype
Some people are born with a thin gum biotype — tissue so delicate that tooth roots are faintly visible through it even in healthy mouths. Thin biotype is one of the strongest predictors of recession even with perfect home care. A related issue is dehiscence — when a tooth erupts outside the bony envelope, there is not enough scaffolding to support stable gum tissue long-term. Family history matters: if a parent has visible recession in their thirties, your risk is meaningfully higher.
4. Malocclusion and occlusal trauma
A tooth that sits outside the arch or takes more bite force than its neighbors concentrates that force at the buccal gum line, and over years the bone and gum migrate down. Common culprits: a rotated lower incisor crowded forward, a high cusp on an unadjusted crown, or a relapsed orthodontic case. Bruxism amplifies everything — sleep forces can be 5–10 times normal chewing force.
If we identify bruxism (worn cusps, flat wear facets, morning jaw soreness), a custom night guard fitted at our Sheepshead Bay office is the most cost-effective intervention to stop progression. For orthodontic causes, clear aligners to move a tooth back into the bony envelope can be a long-term solution.
5. Hormonal changes
Pregnancy gingivitis — swelling and bleeding peaking in the second trimester — can progress to mild recession if home care lapses during morning sickness. Menopause and the drop in estrogen contribute to gingival thinning and underlying osteopenia. The fix is rarely dramatic but does call for cleanings every 3–4 months instead of 6 during these phases.
6. Trauma and iatrogenic causes
The most common iatrogenic cause of focal recession is the tongue or lip piercing. The jewelry sits against a specific tooth for years, and localized recession can become Class III or IV at one tooth in 5–10 years. Other trauma causes: sports impacts without a mouthguard, orthodontic appliance abrasion, and habits like chewing pen caps or nail biting. The first step in treatment is always removing the cause — and yes, that means removing the piercing.
Miller Classification: how dentists grade severity
The Miller classification (Dr. P.D. Miller, 1985) is the standard framework used to grade recession and predict realistic surgical root coverage. Newer systems (Cairo’s RT1/RT2/RT3) are gaining ground in research, but Miller remains the everyday clinical language.
| Miller Class | Recession extent | Interdental tissue | Realistic surgical coverage |
|---|---|---|---|
| Class I | Within attached gum, does not reach mucogingival junction | No bone or papilla loss between teeth | 100% root coverage achievable |
| Class II | Extends past mucogingival junction | No bone or papilla loss between teeth | 100% root coverage achievable |
| Class III | Extends past mucogingival junction | Some bone or papilla loss present | Partial coverage only (typically 50–80%) |
| Class IV | Severe recession on the tooth | Significant bone and papilla loss | Root coverage unrealistic; focus on stopping progression |
The key insight is the interdental papilla — the little triangle of gum between teeth. As long as it is intact (Class I and II), surgeons have a stable framework to graft against and can bring tissue back over the exposed root. Once the bone between teeth is lost and the papilla collapses (Class III and IV), the scaffolding is gone and outcomes become much more limited. This is why early evaluation matters: a Class I problem at age 35 can be fully reversed; the same tooth at Class IV at age 60 cannot.
How to know if your gums are receding (self-assessment)
Most people notice recession either in the mirror or because of new sensitivity. Five quick checks you can do at home:
- Mirror test. Compare the gum line across your front teeth. Is one tooth noticeably “longer” than its neighbor? Do you see a yellowish band of root at the gum line versus the bright white enamel above?
- Tongue test. Run your tongue along the gum line. Does any area feel like a notch or step instead of a smooth transition?
- Sensitivity map. Cold sensitivity from recession is localized to specific exposed roots, not all over. (For all-over sensitivity, see causes and treatment of sensitive teeth.)
- Photo comparison. Recession is slow — compare a recent close-up smile photo to one from 2–3 years ago.
- Floss bleeding. Bleeding from the same spot every time points to inflammation that may be hiding recession.
If any of these raise concern, a periodontal exam is the next step. We measure gum height and pocket depth at six points around each tooth, and the numbers tell us exactly which class is present and whether bone loss is a factor. The exam takes about 20 minutes and is usually fully covered by insurance.
The treatment ladder (matched to severity)
Treatment for recession is always step-wise. Jumping straight to surgical grafting on a patient who still over-brushes is a recipe for losing the graft within 18 months. We work up the ladder, stage by stage.
Stage 1 — Stop the cause
Nothing else works if the driver is still active. This stage is about behavior change: switching to a soft brush (ideally electric with pressure sensor), learning Bass technique, treating bruxism with a night guard, addressing periodontitis if present, and removing piercings. Cost: $20 for a new brush to $595 for a custom night guard. For most patients, this stage alone stabilizes the problem.
Stage 2 — Manage sensitivity and protect exposed roots (Miller I–II without graft)
Once the cause is controlled, the next question is how to manage exposed root surfaces you already have:
- In-office fluoride varnish every 3–6 months (~$45/application). Coats the root, reduces sensitivity, adds caries resistance.
- Prescription-strength fluoride toothpaste at home (5000 ppm formulations like Prevident 5000 Plus), used nightly.
- GC Tooth Mousse or MI Paste after brushing for remineralization.
- Composite bonding to cover the exposed root — typically $225–$485 per tooth. Durable, cosmetic, and shields the root from sensitivity, abrasion, and root cavities. Bonding does not regenerate gum, but it solves the symptom.
For many Class I and small Class II cases not bothering the patient cosmetically, Stage 2 is the final stop. Recession is stopped, sensitivity is managed, surgery is not needed.
Stage 3 — Surgical gum graft (for Class I–III)
When the cosmetic impact is significant, sensitivity is unmanageable, or continued progression threatens the tooth, surgical root coverage becomes the right call. Four main approaches:
- Connective tissue graft (CTG) — the gold standard. Tissue harvested from the palate, placed under a flap raised over the recession site. ~95% root coverage success in Class I/II.
- Free gingival graft (FGG) — thicker palatal tissue grafted directly. Simpler than CTG, predictable for thickening, but less cosmetic.
- Acellular dermal matrix (AlloDerm) — sterile donor tissue, no second surgical site, faster recovery, slightly lower long-term success.
- Pinhole surgical technique (PST) — minimally invasive. Existing gum is loosened through a small pinhole and repositioned over the recession with collagen support. No sutures, no palatal harvest.
Costs typically range from $895 to $1,500 per tooth or treatment area. Most surgical grafting is done by a periodontist (a gum specialist with three additional years of training). Dr. Natalia performs the workup, periodontal exam, Miller classification, and home care planning at our office, and refers to a trusted periodontist for surgery when grafting is indicated. We then handle long-term maintenance.
Stage 4 — Manage when surgery is not realistic (Class IV)
For severe recession with significant bone loss and papilla collapse, surgical root coverage is unlikely to succeed and not usually offered. The path forward is pragmatic:
- Professional cleanings every 3 months to keep inflammation minimal.
- Meticulous home care with adjunct tools (interdental brushes, water flosser, prescription rinse).
- Acceptance that some affected teeth may eventually need extraction.
- Planning ahead for tooth replacement with dental implants in Brooklyn 11229, bridges, or partial dentures.
This is the conversation no one wants, but having it at 55 instead of waiting until a tooth is mobile at 65 produces dramatically better outcomes. We will tell you the truth about what surgery can and cannot do for your case.
When recession is an actual emergency
Most recession is slow and chronic. Once in a while it isn’t. Same-day evaluation is warranted if:
- Recession appears suddenly over weeks rather than years (possible aggressive periodontitis, trauma, or chemical burn);
- A single tooth becomes recessed and loose at the same time (possible abscess or vertical root fracture);
- Recession is accompanied by pus, swelling, or fever (active infection);
- Generalized rapid recession appears without obvious cause (possible systemic factor — diabetes, immunosuppression, medications).
Call (718) 368-3368 the same day for these scenarios.
Four realistic patient scenarios (composite)
Anna, 38, marketing manager from Marine Park. Noticed her lower front teeth looked “longer” in selfies and felt cold sensitivity with iced coffee. Exam: Miller Class I on three lower incisors, thin biotype, hard-bristle manual brush. Plan: electric brush with pressure sensor, Bass technique coaching, fluoride varnish quarterly for 12 months, composite bonding on the most affected tooth. Stable at 18-month follow-up, sensitivity gone.
Robert, 52, electrician. Generalized recession, bleeding gums, persistent bad breath. Probing showed 5–7 mm pockets in every quadrant — moderate generalized periodontitis. Plan: scaling and root planing in two visits, 3-month periodontal maintenance, prescription chlorhexidine. Progression stopped over 9 months. Tooth-replacement planning entered the conversation for two molars with the worst attachment loss.
Yulia, 41, server, lower tongue piercing for 15 years. Localized severe recession on a single lower central incisor (Class II isolated), rest of mouth healthy. Plan: remove the piercing, 8 weeks of soft-tissue healing, then referral for connective tissue graft. At 6 months: ~95% root coverage, sensitivity gone, excellent cosmetic result. The piercing did not go back in.
Boris, 67, retired engineer from Sheepshead Bay. Severe generalized recession, three loose teeth, significant bone loss on bitewings. Class IV across multiple teeth. Surgical root coverage not realistic. Plan: extract the three mobile teeth, immediate transitional partial denture, staged implants over 12 months. We discussed cost openly using the Brooklyn dental insurance guide for 2026 and CareCredit financing.
Common mistakes patients make
- Brushing harder to “clean better.” Pressure does not equal cleanliness. A pressure sensor on an electric brush is the fastest fix.
- Using whitening toothpaste daily for years. The abrasive particles polish away the softer cementum once recession begins. Use intermittently.
- Ignoring bleeding gums. Bleeding is the earliest warning that inflammation is destroying attachment. Schedule a cleaning, not stronger mouthwash.
- Self-treating sensitivity for years. Sensitivity toothpaste masks; if roots are exposed and worsening, you delay the real fix.
- Skipping cleanings to save money. Two cleanings a year prevent the periodontitis that costs ten times more surgically. Our dental cleaning and hygiene program is the highest-leverage spend in your dental budget.
According to the American Academy of Periodontology, more than 47% of American adults over 30 show some form of periodontal disease, and gum recession is among the most common findings on a routine exam. The American Dental Association recommends a comprehensive periodontal evaluation at least once a year.
Prevention (if you don’t have recession yet)
- Soft or extra-soft brush. Electric with a pressure sensor (Sonicare, Oral-B Genius) is the most foolproof option.
- Modified Bass technique: bristles at 45° toward the gum line, short gentle vibrations, no scrubbing.
- Floss daily with proper technique — under the gum, wrap-and-slide, not snap-and-go.
- Cleanings every 6 months (every 3 months with periodontitis history).
- Get evaluated for bruxism if you wake up with jaw soreness or headaches.
- Avoid abrasive whitening pastes as a daily driver.
- Skip tongue and lip piercings.
- Address malocclusion early — a slightly crowded incisor at 25 becomes a recession problem at 45.
When to come to Eco Dental NY
Recession is one of those issues where the timing of the first evaluation matters more than almost any other dental concern. Catch it as Class I, and every option is on the table — including non-surgical management for a lifetime. Wait until Class IV, and the conversation shifts to tooth replacement. We see patients from across Brooklyn — Sheepshead Bay, Marine Park, Midwood, Bensonhurst, Brighton Beach — for periodontal evaluations focused on recession. Dr. Natalia Blazhkevich, DDS (NYU College of Dentistry), personally performs every exam and walks you through realistic options. Our team speaks five languages, which makes the consultation comfortable for patients more fluent in Russian, Polish, Ukrainian, or Uzbek than English. Call (718) 368-3368, learn more about our Sheepshead Bay dental office, or request an appointment online.
Frequently Asked Questions
Can receding gums grow back without surgery?
No. Once gum tissue has receded, it does not regenerate on its own. What can happen is that inflamed, swollen gums can become less swollen with good home care and look slightly “fuller” — but the actual tissue that was lost does not come back. The only way to genuinely restore lost gum tissue over a root surface is surgical grafting, and that only works for Miller Class I, II, and some Class III cases. The realistic non-surgical goal is to stop further progression and manage symptoms.
How much does a gum graft cost in Brooklyn?
Gum graft cost typically ranges from about $895 to $1,500 per tooth or per treatment area, depending on technique (connective tissue graft, pinhole, AlloDerm) and case complexity. Multiple adjacent teeth treated together are often discounted. Insurance with periodontal coverage may pay 50–80% if the procedure is deemed medically necessary. We provide a written estimate after the exam so you know the exact out-of-pocket number before scheduling.
Does dental insurance cover gum graft?
Most PPO plans with periodontal coverage will pay some portion of a gum graft when there is documented attachment loss and the procedure is medically necessary (not purely cosmetic). Coverage typically ranges from 50% to 80% after deductible. Plans without periodontal benefits will not cover it. We verify benefits in advance and submit pre-authorization for surgical procedures so there are no surprises. See our Brooklyn dental insurance guide for 2026 for plan-by-plan detail.
How long does gum graft healing take?
Initial soft-tissue healing takes about 2 weeks, during which you eat soft foods and avoid brushing the grafted area. Most patients return to normal eating by 3–4 weeks. Full tissue remodeling and color match takes 3–6 months, and the long-term result is evaluated at 6 months. The palate donor site (for CTG and FGG) typically heals in 2–3 weeks with a protective putty placed at surgery.
Is laser treatment better than traditional gum graft?
For recession specifically — restoring tissue over an exposed root — lasers are not a replacement for grafting. Lasers (LANAP and similar) treat periodontitis pockets, not recession defects. Some clinicians use lasers as a hemostasis adjunct during graft surgery, but the graft itself still uses connective tissue, free gingival tissue, or a dermal matrix. Be skeptical of anyone advertising a laser-only solution for moderate recession.
Can I prevent further recession at this stage?
Yes, in almost every case. The single most important step is identifying and removing the underlying cause — over-brushing, periodontitis, bruxism, malocclusion, or trauma. Once the cause is controlled, the rate of further recession typically drops by 80% or more. Twice-yearly periodontal exams with measurements catch any progression before the next class transition.
At what point should I see a periodontist versus my general dentist?
Start with your general dentist. We perform the workup, periodontal exam, Miller classification, and risk-factor analysis. For stable Class I cases, no specialist visit is needed — we manage them in-house. For surgical grafting (most Class II and many Class III), we refer to a board-certified periodontist with whom we have a long-standing relationship. We handle pre-op planning and post-op maintenance; the periodontist handles the surgery itself.
Can mouthwash help with receding gums?
Mouthwash is an adjunct, never a primary treatment. Antimicrobial rinses (chlorhexidine, essential-oil based) reduce bacterial load when recession is tied to gum disease, and fluoride rinses help desensitize exposed roots. But no mouthwash thickens tissue, regrows attachment, or covers roots. Use it as one piece of a broader plan, not as the plan.
Book Your Visit to Eco Dental NY
Dr. Natalia Blazhkevich, DDS — sole provider, 5 languages spoken (English, Russian, Polish, Ukrainian, Uzbek). 2384 Ocean Avenue, STE 1, Brooklyn, NY 11229. Call (718) 368-3368 or request an appointment online. Mon–Fri 9 am – 7 pm.