Dental care during pregnancy is not just safe — it is actively recommended by the American College of Obstetricians and Gynecologists (ACOG) and the American Dental Association (ADA). Yet roughly half of pregnant women skip routine dental visits, often because of outdated myths their grandmother (or the internet) passed down. This 2026 Brooklyn guide explains, in plain language, exactly what is safe at our practice, what we defer until after delivery, and which trimester is the best window for any work you genuinely need.
Why this guide exists
Most pregnant women in Brooklyn arrive at our Sheepshead Bay office with one of two beliefs: either “I cannot have any dental work until after the baby comes” or “I am too scared to ask my dentist what is okay.” Both lead to the same outcome — postponed cleanings, ignored toothaches, and small problems that grow during a time when your body is already under remarkable demand.
The medical consensus has been settled for more than a decade. ACOG’s formal Committee Opinion states that “oral health care during pregnancy is safe and should be recommended.” The ADA echoes this. At our single-dentist Brooklyn practice, founded in 2018, we see roughly thirty pregnant patients each year — and the conversation almost always begins with relief once they hear what is actually safe.
Dr. Natalia Blazhkevich, our sole provider, treats every pregnant patient personally. As a female dentist trained at NYU College of Dentistry, she understands that pregnancy is not a medical event to defer your mouth through — it is a season in which your oral and obstetric health are closely linked. Untreated dental infections are associated with preterm birth and low birth weight in multiple peer-reviewed studies. Doing nothing is rarely the safe option.
The big-picture safety framework
Three professional bodies — ACOG, the ADA, and the American Academy of Periodontology — converge on the same conclusions. Routine dental care is safe at any point during pregnancy. Necessary treatment for active disease should not be delayed. Elective cosmetic procedures are reasonable to defer, not because they are dangerous, but because they are non-urgent.
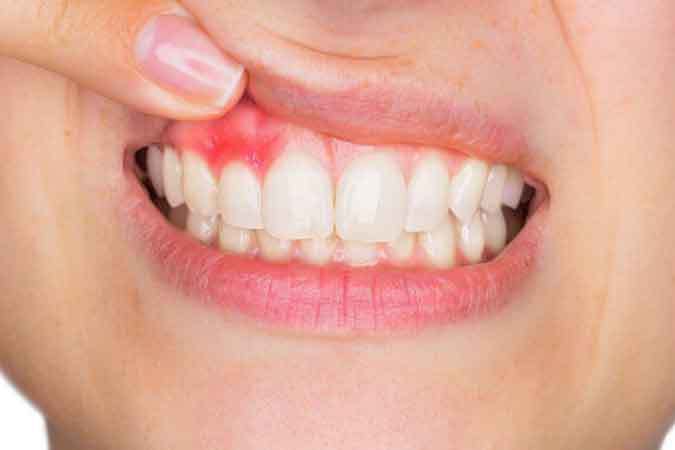
Pregnancy hormones — particularly the surge in progesterone and estrogen — change how your gums respond to the bacteria already present in your mouth. The result is “pregnancy gingivitis,” affecting an estimated 60 to 75 percent of pregnancies. Untreated, it can progress to periodontitis — and periodontitis, unlike gingivitis, is the form genuinely linked to adverse pregnancy outcomes. The takeaway: you are not protecting your baby by skipping the dentist. In most cases, you are doing the opposite.
What is SAFE during pregnancy
The list below reflects standard-of-care dentistry as practiced at our Sheepshead Bay office, consistent with ACOG and ADA guidance. None of these procedures requires waiting until after delivery.
- Routine cleanings and periodontal cleanings — every trimester. In fact, more frequent cleanings (every three to four months) are often recommended during pregnancy. See our cleaning and hygiene program for what a visit looks like.
- Comprehensive dental exam — any trimester.
- Bitewing X-rays with a lead apron and thyroid collar (radiation numbers explained below).
- Composite fillings — with local anesthetic, any trimester (second trimester preferred).
- Root canals — when infection is present, treatment is safer than waiting. Visit our root canal page for what to expect.
- Periodontal scaling and root planing — for active gum disease, any trimester.
- Tooth extraction — when necessary, ideally in the second trimester.
- Bonding repairs for chipped or fractured teeth — any trimester.
- Crown placement for broken or decayed teeth that cannot be saved with a filling — second trimester preferred.
- Local anesthetic (lidocaine 2% with epinephrine 1:100,000) — long-established safety profile.
- Antibiotics from the pregnancy-compatible group (amoxicillin, penicillin, cephalexin, clindamycin) when bacterial infection is present.
- Emergency care for acute pain, swelling, or trauma — at any point in pregnancy. Please do not wait. See our severe tooth pain emergency page.
What to DEFER until after delivery
This list is shorter, and the reasoning matters. We defer these treatments not because they are dangerous to you or your baby, but because they are non-urgent. Pregnancy is a reasonable time to minimize any avoidable intervention, and almost all of these procedures will give a better result with better comfort once your body is no longer in pregnancy mode.
- Teeth whitening — both in-office and take-home. Peroxide safety data in pregnancy is limited; the procedure is purely elective. Wait.
- Porcelain veneers — multi-appointment cosmetic work with no urgency.
- Elective Invisalign starts — see the FAQ below if you are already mid-treatment when pregnancy begins.
- Wisdom tooth extraction when the tooth is asymptomatic. If infected or causing pain, we treat in the second trimester.
- Dental implant placement (the surgical phase) — unless replacing a tooth lost to trauma.
- Nitrous oxide sedation — we do not use nitrous oxide during pregnancy at our practice. The first-trimester data is concerning; second and third trimesters remain debated.
- Oral conscious sedation (Halcion, triazolam) — avoid entirely during pregnancy.
- IV sedation — avoid entirely during pregnancy.
- Long single appointments over one hour in the third trimester — broken into shorter visits to avoid supine positioning fatigue.
What this means practically: If you are pregnant and we discover a small cavity, we restore it. If you are pregnant and want whiter teeth for maternity photos, we book you for whitening after your six-week postpartum checkup. The dividing line is necessity, not anxiety.
Optimal treatment timing by trimester
If you have a choice about when to schedule dental work, the second trimester is the answer. The reasons are practical: organogenesis (fetal organ development) is largely complete, you are typically past the nausea peak, you can still lie comfortably in a dental chair, and you are not yet experiencing the supine-position fatigue of the third trimester.
First trimester (weeks 1–13)
Routine cleanings: yes, fully recommended.
Emergency restorative work: yes, when necessary — toothaches and infections do not wait.
Elective work: defer to the second trimester or post-delivery.
Why the caution: the first trimester is when the baby’s organs are forming. Even though local anesthesia and shielded X-rays show no evidence of harm, we use this window only for cleanings and genuine clinical need.
Second trimester (weeks 14–27) — the optimal window
All necessary dental work can be performed comfortably. Patients are typically past morning sickness, the baby’s major organ development is complete, and you can still lie back in the chair without compression issues. If you know you need fillings, a crown, or a root canal, this is when we schedule them. Many of our pregnant patients come in for a “second-trimester catch-up” around weeks 16 to 22 to handle anything that has been quietly developing.
Third trimester (weeks 28–40)
Routine cleanings: yes, with modified positioning.
Emergencies: treated promptly with adjustments.
Long appointments: avoided when possible — we break work into shorter visits.
Chair positioning: we use a left-side tilt and semi-upright posture to prevent the uterus from compressing the inferior vena cava, which can cause dizziness and lower blood pressure.
Pregnancy gingivitis — the most common dental issue you will face
Sixty to seventy-five percent of pregnancies are affected. If your gums have started bleeding more easily, swelling slightly, or turning redder than before — that is the diagnosis, and it is so common we treat it as an expected part of prenatal dental care, not a complication.
The mechanism is hormonal, not behavioral. Even patients with excellent home care develop pregnancy gingivitis, because hormones change how gum tissue responds to plaque bacteria that have always been there. Symptoms usually appear between months two and eight, peak in the third trimester, then resolve within a few months of delivery — provided you do not let it progress.
How we treat it at Eco Dental NY
- More frequent professional cleanings: every three to four months instead of the usual six.
- Gentle home care: soft-bristled brush, twice daily, two minutes each time. Aggressive brushing makes bleeding worse, not better.
- Daily flossing: critical. The bacterial film between teeth is where gingivitis lives. Skipping floss during pregnancy makes the problem dramatically worse.
- Alcohol-free antimicrobial rinse: chlorhexidine 0.12% when clinically indicated, used short-term.
- Nutritional support: vitamin C and folate from food sources support gum tissue resilience.
If pregnancy gingivitis is left untreated through the entire pregnancy, it can progress to periodontitis — and unlike gingivitis, periodontitis is the form independently associated with preterm birth and low birth weight in clinical research. This is the single biggest reason we ask pregnant patients to come in every three to four months rather than every six.
Pregnancy tumors (pyogenic granuloma of pregnancy)
About 0.5 to 5 percent of pregnancies produce a small, soft, red growth on the gum — most often on the upper jaw between two teeth. The medical name is pyogenic granuloma of pregnancy, sometimes called “epulis gravidarum.” The word “tumor” alarms patients, but these are benign and unrelated to cancer. They are typically painless, sometimes bleed when brushed, and around 85 percent resolve on their own within weeks of delivery. We monitor them through pregnancy and only consider surgical removal if the growth interferes with eating or bleeds persistently — generally postponed until after delivery.
Dental X-rays during pregnancy — the actual numbers
This is the single most-asked question we hear from expectant mothers, so let us put real numbers on the page.
| Exposure source | Radiation dose (mSv) |
|---|---|
| Four bitewing dental X-rays (with shielding) | ~0.005 |
| Single panoramic dental X-ray | ~0.014 |
| Full-mouth dental series (18 films) | ~0.04 |
| Daily background radiation (just from living) | ~0.008 per day |
| Cross-country airplane flight | ~0.03 |
| Threshold for any documented fetal harm | 50 – 100 |
Read that bottom row again. The dose at which any fetal harm has ever been documented in research is 50 to 100 millisieverts. A complete set of four bitewing dental X-rays delivers 0.005 millisieverts — roughly one ten-thousandth of the lower threshold. A single dental bitewing exposes the fetus to less radiation than you receive simply by walking around outside for a few hours.
We always use a lead apron with a thyroid collar for any pregnant patient who requires imaging, and we only take X-rays when the clinical need outweighs even this minimal exposure. The science is unambiguous: shielded dental X-rays during pregnancy have effectively zero radiation risk to the developing baby.
Anesthesia choices during pregnancy
Anxiety about anesthesia is the second-most-asked question, and again the answer is more reassuring than the rumor mill suggests.
- Lidocaine 2% with epinephrine 1:100,000 — our first-choice local anesthetic. Pregnancy Category B, decades of safety data, what most pregnant patients receive.
- Articaine 4% — similar safety profile, used when lidocaine is not ideal for the specific tooth or anatomy.
- Topical anesthetic gels (benzocaine, lidocaine spray) — safe in normal clinical doses applied briefly to gum tissue.
- Mepivacaine — we generally avoid in pregnancy due to less robust safety data.
- Nitrous oxide (“laughing gas”) — we do not use during pregnancy. First-trimester exposure data is concerning; second and third trimester use remains debated in the literature. Avoiding it costs the patient nothing.
- Oral sedation (Halcion, triazolam) — avoid entirely.
- IV sedation — avoid entirely. If you have severe dental anxiety, please read about our non-pharmacological anxiety management approach, which works well during pregnancy.
The epinephrine in local anesthetic occasionally raises concern. The dose used in a dental injection is tiny — 0.018 milligrams in a typical cartridge — and the body produces far more endogenous epinephrine during normal stress. There is no clinical evidence that the epinephrine in standard dental anesthetic causes harm during pregnancy.
Pain medications by trimester
What you take at home for a toothache matters more during pregnancy than at any other time. Here is the framework we give our patients:
| Medication | 1st trimester | 2nd trimester | 3rd trimester |
|---|---|---|---|
| Acetaminophen (Tylenol) | Safe — first choice | Safe — first choice | Safe — first choice |
| Ibuprofen / NSAIDs | Use with caution; brief course only | Use with caution; brief course only | AVOID — risk of premature closure of fetal ductus arteriosus |
| Aspirin | Avoid for pain | Avoid for pain | Avoid |
| Opioids (codeine, hydrocodone) | Last resort, brief | Last resort, brief | Last resort, brief |
Acetaminophen is the first-line pain medication for dental pain throughout pregnancy — maximum 3,000 to 4,000 milligrams in any 24-hour period, at the lowest effective dose for the shortest time needed. If you have a toothache during pregnancy, do not silently swallow ibuprofen because it is what you used pre-pregnancy. Reach for acetaminophen, and call us. Most dental pain has a fixable underlying cause.
Common patient questions, with our actual answers
“I have a tooth infection — should I just wait until after delivery?”
No. Untreated dental infections release bacteria and inflammatory molecules into the bloodstream, and research links untreated maternal periodontal infection to preterm birth and low birth weight. Treating with a root canal or extraction is safer than waiting. We schedule in the second trimester when possible; if pain or swelling is acute, we treat at any point.
“My gums bleed every time I brush — should I just stop?”
No. Stopping brushing allows plaque to accumulate, worsening the inflammation that is making your gums bleed. Continue brushing gently with a soft-bristled brush twice daily, floss daily, and schedule a cleaning. The bleeding stops within days to weeks of treatment.
“Can my baby take calcium from my teeth?”
No. The old “you lose a tooth per baby” saying is folklore, not medicine. The calcium in your teeth is fixed in mineralized enamel and does not dissolve into your bloodstream to feed the baby. Pregnancy gingivitis can damage gum and supporting bone if untreated, but the mechanism is inflammation, not calcium theft.
“What if I need wisdom teeth out?”
If the wisdom tooth is asymptomatic, we wait until after delivery. If it is infected — pericoronitis with swelling, pain, or trismus — we treat in the second trimester whenever possible, with local anesthesia only and a short appointment. Severe infections are themselves a pregnancy risk and cannot simply be deferred.
When to come see us at Eco Dental NY
If you are pregnant or planning pregnancy in Brooklyn, here is the simple framework. Schedule a cleaning and exam early — ideally in your first trimester or even before conception if you are still in the planning phase. Tell us your due date. We will set a treatment plan that handles necessary work in the second trimester, schedules cleanings every three to four months for pregnancy gingivitis prevention, and defers anything cosmetic until after you have recovered from delivery.
Dr. Natalia personally sees every pregnant patient at our practice. Many of our expectant moms tell us they appreciate having a female dentist who understands pregnancy from both clinical training and lived professional experience — a small detail that makes the appointment feel less clinical and more like a conversation between adults. We have served Brooklyn since 2018 from our office at 2384 Ocean Avenue, just off Sheepshead Bay, and our team speaks five languages: English, Russian, Polish, Ukrainian, and Uzbek.
Coverage is rarely a barrier. We accept eighteen PPO plans plus Medicaid (including HealthFirst, Affinity, AmeriGroup, EmblemHealth, and MetroPlus), 1199SEIU benefits, and offer CareCredit financing. Pregnant women on Medicaid in New York have full dental coverage including cleanings, fillings, extractions, and root canals — see our 2026 Brooklyn insurance guide for details. Patients across Sheepshead Bay, Marine Park, Midwood, and Brighton Beach come to us specifically for pregnancy-aware care.
Frequently Asked Questions
Can I whiten my teeth during pregnancy?
We recommend deferring all teeth whitening — both in-office and take-home — until after delivery and, if breastfeeding, until you have finished. The peroxide gel used in whitening has limited safety data in pregnancy, and whitening is purely cosmetic with no urgency. Most patients who whiten for maternity photos end up happier whitening after delivery anyway, since pregnancy hormones can cause temporary gum sensitivity that makes whitening less comfortable.
Is fluoride safe during pregnancy?
Yes. Standard fluoride toothpaste (1,000–1,500 ppm) and fluoride in public drinking water are safe during pregnancy and may even benefit fetal tooth development. The ADA and ACOG both support continued fluoride use during pregnancy. We do not recommend exceeding normal amounts — swallowing large quantities of toothpaste is not advised — but normal twice-daily brushing is exactly what you should be doing.
Should I switch toothpaste during pregnancy?
If morning sickness makes the taste of your usual toothpaste trigger nausea, switch to a milder flavor. Avoid toothpastes with strong whitening or charcoal additives. Otherwise, a standard fluoride toothpaste is fine. Some patients brush with just water during the worst nausea weeks and rinse with fluoride mouthwash later in the day.
Can I get Invisalign while pregnant?
If you are already in active Invisalign treatment, you can almost always continue — the aligners are inert plastic and pose no risk. We typically pause cosmetic refinement attachments or IPR (interproximal reduction) until after delivery. For new starts, we generally recommend waiting until after delivery. See our Invisalign page for details.
What about dental X-rays in the first trimester?
We avoid routine X-rays in the first trimester not because they are dangerous — the dose is far below any harm threshold — but because routine imaging can usually wait until the second trimester. Emergency X-rays for trauma, severe pain, or suspected infection are taken in any trimester when clinically necessary, always with a lead apron and thyroid collar.
Does Medicaid cover dental care during pregnancy in New York?
Yes. New York State Medicaid covers comprehensive dental care for pregnant women — cleanings, exams, X-rays, fillings, extractions, and root canals. Pregnant women often qualify for expanded Medicaid during pregnancy and for sixty days postpartum, even if they were not previously enrolled. We accept all major Medicaid managed care plans.
Is local anesthesia really safe for the baby?
Yes. Lidocaine with epinephrine is the most-studied local anesthetic in human pregnancy and has decades of safety data. It is FDA Pregnancy Category B and is the same medication used by obstetricians for procedures during pregnancy. The amount delivered in a dental injection is tiny — typically under 0.04 grams of lidocaine — and acts locally rather than systemically. Untreated dental infection poses substantially more risk than a properly administered local anesthetic.
I’m planning to get pregnant — should I do dental work now?
Yes — one of the smartest moves you can make. A pre-conception dental checkup lets us complete cosmetic work, replace old fillings, treat any subclinical gum issues, and create a clean baseline before pregnancy hormones change the landscape. Patients who enter pregnancy with a healthy mouth experience less pregnancy gingivitis and fewer dental emergencies. If you are planning, please book a comprehensive exam now.
Book Your Visit to Eco Dental NY
Dr. Natalia Blazhkevich, DDS — sole provider, 5 languages spoken (English, Russian, Polish, Ukrainian, Uzbek). 2384 Ocean Avenue, STE 1, Brooklyn, NY 11229. Call (718) 368-3368 or request an appointment online. Mon–Fri 9 am – 7 pm. Expectant mothers welcome at any stage of pregnancy — please mention your due date when booking so we can plan your care around the optimal trimester window.