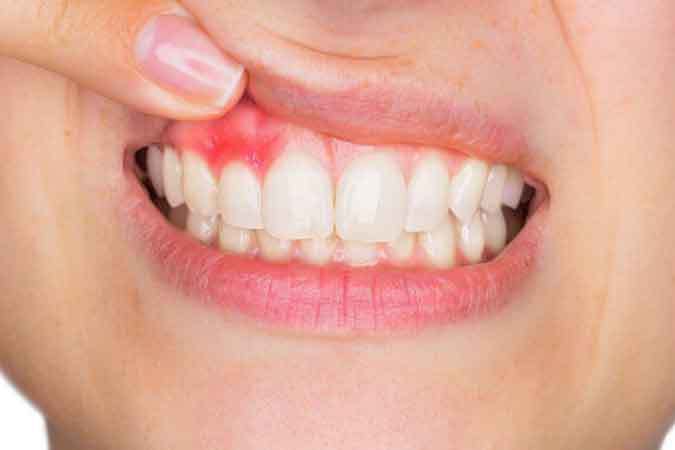
Dental abscess: 7 signs you need same-day emergency treatment
A dental abscess is a bacterial infection that can spread fast. Know the signs, what NOT to do, and when to come in same-day vs. when to go to an ER.
- ★★★★★ 4.8 from 90+ Google reviews
- NYU DDS
- Walk-ins welcome
- 5 languages
- Mon-Fri 9am-7pm
What a dental abscess actually is
A dental abscess is a localized collection of pus caused by a bacterial infection. The infection usually starts from one of two places: (1) inside a tooth where decay has reached the nerve (a periapical abscess), or (2) in the gum pocket alongside a tooth (a periodontal abscess).
The reason an abscess is a true dental emergency is not just the pain — it is that the infection can spread. In the head and neck, bacteria can travel along anatomical pathways into the soft tissues of the face, neck, and (rarely but seriously) the airway or brain. This is why dentists treat abscesses urgently and why some cases need to go to an ER instead of a dental office.
The 7 warning signs
If you have any of these, do not wait:
- Throbbing, persistent pain. Often worse at night. Different from a cavity ache — this is deeper, constant, and gets worse with biting.
- Pus or foul taste in your mouth. You may see a “pimple” on the gum (this is a fistula draining the abscess) — its appearance is a warning even if pain is mild.
- Swollen, tender gum around the tooth. Red, puffy, warm to touch.
- Facial swelling. One side of your face is visibly bigger than the other. This is a sign the infection is spreading beyond the gum.
- Fever, chills, or generally feeling sick. A bacterial infection significant enough to cause systemic symptoms needs prompt treatment.
- Swollen lymph nodes under your jaw or in your neck. Your immune system is fighting the infection — also a spread signal.
- Sensitivity to hot, cold, or biting pressure that’s much worse than usual. The nerve is dying or already dead.
Go to ER, not a dentist, if
⚠ Hospital ER warning signs (call 911 or go to ER immediately)
- Facial swelling is spreading rapidly
- Difficulty breathing or swallowing
- Stiff neck or trouble opening your mouth
- High fever (above 102°F / 38.9°C) with chills
- Eye swelling shut on the same side as the infection
- Visible swelling under the tongue
These are signs of Ludwig’s angina or other deep-space infections. They are rare but life-threatening. A dental office is not equipped to manage these — ER first, then dental follow-up.
Closest 24-hour ERs to Sheepshead Bay: NYU Langone Brooklyn (150 55th St), Maimonides Medical Center (4802 10th Ave), Coney Island Hospital (2601 Ocean Pkwy).
What we do for an abscess at Eco Dental NY
For a non-airway-threatening abscess seen during our hours (Mon-Fri 9am-7pm):
- Quick clinical exam + X-ray to identify the source tooth and the extent of the infection.
- Pain control. Local anesthesia to numb the area before any work.
- Drainage. We open the abscess so the pus can drain out — relieving pressure immediately. This is when most patients feel immediate relief.
- Antibiotic prescription. Usually amoxicillin (or clindamycin if you’re allergic to penicillin). 7-10 day course.
- Definitive treatment plan. Antibiotics + drainage stop the infection but don’t fix the underlying problem. We either need to do a root canal on the tooth, or extract it. We discuss both options with you.
- Follow-up appointment scheduled. Usually within 48-72 hours after the antibiotics take effect.
What NOT to do with an abscess
- Don’t apply heat. Heat increases blood flow to the area and helps bacteria multiply. Use cold compresses if anything.
- Don’t try to lance it yourself. Without sterile conditions and anesthesia, you’ll cause more damage and risk spreading the infection.
- Don’t rely on antibiotics alone. They control the infection temporarily but the tooth still needs definitive treatment (root canal or extraction). Stopping antibiotics without follow-up almost always means the abscess returns.
- Don’t ignore it because the pain went away. Sometimes the nerve dies and pain disappears — but the infection is still there and still spreading.
Frequently asked questions
Will antibiotics alone cure my dental abscess?
No. Antibiotics control the bacterial infection temporarily but they do not cure the underlying problem — a dead nerve or infected gum pocket. The tooth still needs definitive treatment (root canal or extraction). Antibiotics without follow-up almost always means the abscess comes back.
Can a dental abscess kill you?
Extremely rarely. In modern healthcare, deaths from dental infections are vanishingly rare because antibiotics and drainage are widely available. The serious risks come from deep-space infections (Ludwig’s angina, cavernous sinus thrombosis) which require hospital-level care — that’s why we say go to ER for spreading facial swelling or breathing trouble.
How much does abscess treatment cost?
Initial emergency exam + X-rays: $150-200. Drainage + antibiotic prescription: $200-400. Follow-up root canal: $800-1,600 (or extraction: $200-700). Medicaid and most insurance plans cover these procedures.
Can I take ibuprofen for an abscess until I can see you?
Yes. Ibuprofen 400-600 mg every 6 hours helps with pain and reduces inflammation. Acetaminophen (Tylenol) is also fine but less effective for dental pain.
Do you accept Medicaid for emergency abscess treatment?
Yes. We accept HealthFirst, Affinity, AmeriGroup, EmblemHealth, MetroPlus Medicaid and 1199SEIU. Emergency procedures are typically fully covered.
How fast can you see me for an abscess?
If you call (718) 368-3368 first thing in the morning Mon-Fri, you’ll usually be seen within 2-3 hours. Same-day capacity is reserved every weekday.
Get same-day emergency care now
Mon–Fri 9am–7pm. Walk-ins welcome. Russian, Polish, Ukrainian spoken. Medicaid + 18 insurance plans accepted.
Related emergency dental topics
Find a dentist by Brooklyn ZIP code
Eco Dental NY serves 8 southern Brooklyn ZIP codes. Click your ZIP for area-specific information.